Healthcare Professionals
Pain and Recovery Resources
Within each area you will find links to download and read the resources, which include patient information, publications, clinician training and videos.
You can access these resources by scrolling down this page and selecting the resource you require from the buttons below.

- Pain App
- Physio Review
- NHS Decision Support Tools
- Stoma Support
Keele Pain Recorder App
The Keele Pain Recorder (KPR) is a mobile application (app) which was developed by patients for patients.
The app has undergone clinical trials and been subject to scientific evaluation. It records your level of pain, how this interferes with your life, mood, and sleep on a daily or weekly basis. It records how medication is helping your condition, or if you experience side effects. This can be shared with your doctor to help treat your condition via Email or through the app itself.
With support from the West Midlands Academic Health Science Network (WMASHN)(http://www.wmahsn.org/) and Stoke-on-Trent Clinical Commissioning Group (https://www.stokeccg.nhs.uk/) the KPR is freely available to all pain sufferers.
Download via Google Play or on the Apple app store by clicking on the box below.
Dr John Bedson introduces the Keele Pain Recorder (KPR)
And describes its benefits for patients managing pain
Review of Physiotherapy Research
Musculoskeletal conditions (pain in the joints, ligaments, muscles, nerves, tendons) are the leading cause of pain and disability in the UK, affecting more than 10 million people.
These conditions can have a huge impact on a person’s quality of life, as well as affecting their family, friends, carers and the wider society. Published in 2018, the National Institute for Health and care Research’s Themed review, ‘Moving Forward: Physiotherapy for Musculoskeletal Health and Wellbeing’, brings together high quality research from over the past decade, with the aim to give a clear direction to patients, physiotherapists, researchers, commissioners and planners of physiotherapy and musculoskeletal services.
The research featured in Moving Forward clearly showed that early access to physiotherapy services, exercise, activity and self-management advice can improve patient outcomes, reduce healthcare costs and reduce the need for further investigations and treatments.
However, the full version is complex, it’s 64 pages long and includes over 50 studies, so we created a public version of the Moving Forward Review. The public version aims to empower physiotherapists and patients to work together to improve their quality of life and manage their MSK conditions using best evidence.
The public version is below and the full version is further down the page.
Moving Forward Public Version
Moving Forward Full Version
NHS Decision Support Tools
Shared decision making is a fundamental component of personalised care and is an ethical, professional and medico-legal standard for health and care related decision making.
Decision support tools are one way of facilitating this process, and aim to encourage patients to be more involved in their care planning. Decision support tools can help patients and clinicians to work together to decide on the best course of action for their condition. They encourage conversations about evidence based management options and the potential risks and benefits. They ensure that patient values, preferences and circumstances are taken into account when planning next steps.
Currently we would recommend that these tools are used universally with people with the following conditions:
Knee osteoarthritis; Hip osteoarthritis; Carpal tunnel syndrome; Dupuytren’s contracture.
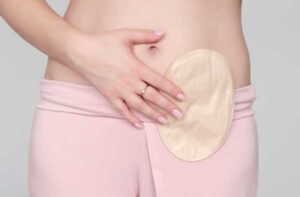
Stoma Support
The video below features Megan, Sahara and Lucy, who discuss their experiences of stoma surgery, their advice to young people undergoing stoma surgery in the future, and their experiences of advising on the research. It can be a useful resource for young people awaiting on contemplating having stoma surgery, and for healthcare professionals working with this patient group, who can signpost their young patients to this resource for peer support, information and reassurance.
The video has been devised through the Stoma Support Study, led by Dr Ben Saunders, which was carried out at Keele University and funded by the NIHR School for Primary Care Research (SPCR). Researchers collaborated with young people who have inflammatory bowel disease (IBD) and a stoma, and a multidisciplinary group of healthcare professionals (HCPs), to co-design a digital intervention to support the management of distress experienced by young people after stoma surgery. The intervention comprises two components: a) a brief training package for HCPs to enhance identification and management of stoma-related distress; and b) a resource to by accessed by young people to support them to self-manage and reduce distress. Throughout the study researchers worked closely with a Patient and Public Involvement and Engagement group of nine young people with IBD and a stoma, who advised on all aspects of the research.